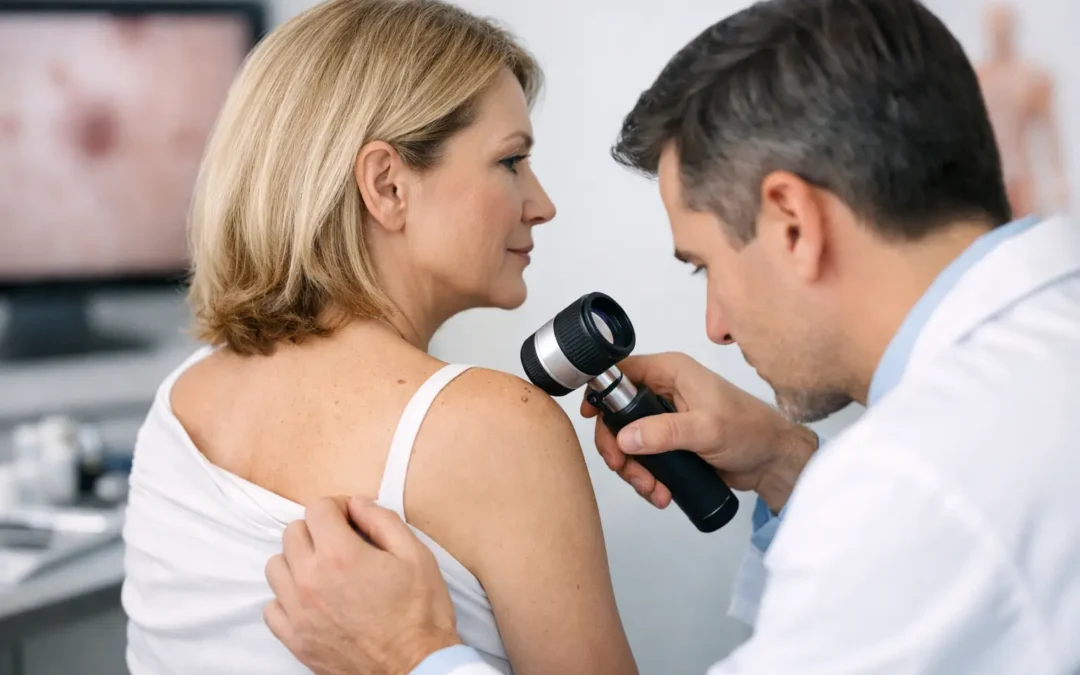
A spot that looked like a freckle last summer now seems darker, a little irregular, and hard to ignore. That is usually when people start searching for a skin cancer screening dermatologist – not because they want a lecture, but because they want a clear answer.
A professional skin exam is one of the most practical steps you can take to protect your health. Skin cancer is common, and early detection can make treatment simpler and more effective. The challenge is that many concerning lesions do not always look dramatic. Some are subtle. Some resemble harmless age spots, pimples, or scars. That is where a board-certified dermatologist adds real value.
Why a skin cancer screening dermatologist matters
A full-body skin exam is not just a quick glance at a few moles. A dermatologist is trained to evaluate patterns, pigmentation changes, texture differences, and lesion behavior in ways that are difficult to replicate at home. Even people who are careful about sunscreen can develop skin cancer, especially if they have a history of sun exposure, tanning bed use, fair skin, or a family history of melanoma.
There is also a practical reason to see a specialist instead of waiting. Skin cancers do not all behave the same way. Basal cell carcinoma often grows slowly, but it can still damage nearby tissue if left untreated. Squamous cell carcinoma may become more aggressive over time. Melanoma is the one most people worry about, and for good reason – it can spread quickly if not caught early.
A skin cancer screening dermatologist is looking for more than obvious warning signs. They are also tracking changes over time and identifying lesions that deserve closer evaluation before they become more serious.
When you should schedule a skin check
Some patients benefit from annual exams, while others need more frequent monitoring. It depends on personal risk factors, skin type, medical history, and whether you have had suspicious lesions before.
You should strongly consider scheduling a screening if you have many moles, a personal or family history of skin cancer, frequent sun exposure, a history of blistering sunburns, or a changing spot anywhere on the body. Screening is also worth discussing if you have a lesion that bleeds, crusts, does not heal, or keeps returning after seeming to improve.
Age matters, but not in the way many people assume. Skin cancer risk increases over time, yet younger adults can develop melanoma as well. Children and teens may not need routine screening in the same way high-risk adults do, but any new or unusual lesion should still be evaluated promptly.
For busy families and working adults, one of the biggest barriers is timing. People delay care because the lesion does not hurt or because they are unsure whether it is serious enough. In dermatology, waiting for pain is not a good strategy. Many skin cancers are painless in the early stages.
What happens during a skin cancer screening dermatologist visit
Patients often expect the appointment to be uncomfortable or complicated. In reality, a screening visit is usually straightforward and efficient.
Your dermatologist will review your personal and family history, including any past skin cancers, severe sunburns, tanning bed exposure, or immune system concerns. From there, a full-body exam is performed to inspect the skin from head to toe. This includes areas patients often overlook, such as the scalp, ears, back, soles of the feet, and between the toes.
If a lesion stands out, the dermatologist may examine it more closely with a dermatoscope, a handheld tool that helps visualize structures beneath the skin surface. Not every suspicious-looking spot requires immediate removal, but some do need a biopsy. A biopsy is the only way to confirm whether a lesion is cancerous or precancerous.
That can sound intimidating, but it is often a simple in-office procedure. The next steps depend on the findings. Some lesions only need monitoring. Others may require treatment ranging from topical therapy or cryotherapy to excision or Mohs surgery, depending on the diagnosis and location.
What you can do before your appointment
A little preparation helps make the exam more useful. If possible, remove nail polish and avoid heavy makeup so the dermatologist can clearly assess the skin. Make note of any spots that are new, changing, itchy, bleeding, or otherwise different from the rest. If you have older photos that show how a mole has changed, bring that information with you.
It is also helpful to know your family history. Even a basic understanding of whether a parent or sibling had melanoma or another skin cancer can guide how often you should be screened.
Patients sometimes worry about overreacting. The better approach is to think of screening as preventive care, not a worst-case scenario. A normal exam can provide reassurance. An abnormal finding can lead to earlier treatment, which is often less extensive than treatment for a neglected lesion.
Signs that should not wait for your next routine exam
Regular screening is valuable, but some changes deserve prompt attention instead of waiting for an annual visit. A mole that becomes asymmetric, develops an uneven border, changes color, grows noticeably, or starts evolving in any way should be evaluated. The same is true for a sore that does not heal, a pearly bump, a rough scaly patch, or a growth that repeatedly bleeds.
The classic ABCDE rule for melanoma can still be helpful: asymmetry, border irregularity, color variation, diameter, and evolving appearance. But real life is not always textbook. Some dangerous lesions do not fit neatly into those categories. If one spot looks different from your other moles – the so-called ugly duckling sign – that alone is reason to have it checked.
Why at-home checks still matter
A professional exam does not replace monthly self-checks. It works best alongside them.
Most people notice skin changes in between visits, not during them. Taking a few minutes each month to look over your skin can help you catch changes earlier. Use a mirror for hard-to-see areas, and ask a partner or family member to help with the scalp or back if needed.
That said, self-checks have limits. It is easy to miss subtle warning signs or dismiss a lesion that seems minor. A dermatologist brings pattern recognition, diagnostic tools, and clinical experience that home monitoring cannot replace.
Screening frequency is not one-size-fits-all
One of the most common questions is how often to schedule a skin exam. The answer depends.
For some patients, yearly screening is appropriate. For others with a history of melanoma, multiple atypical moles, significant sun damage, or previous nonmelanoma skin cancers, visits may be recommended more often. Patients who are immunosuppressed can also need closer follow-up because their risk profile is different.
This is where individualized care matters. A thoughtful dermatologist will not apply the same schedule to every patient. The goal is to match screening frequency to actual risk while keeping care practical and manageable.
Choosing the right dermatology practice
If you are looking for a skin cancer screening dermatologist, credentials and access both matter. Board-certified dermatologists are trained to identify suspicious lesions, perform biopsies, and recommend evidence-based treatment. If skin cancer is diagnosed, it is helpful to have access to a practice that can coordinate the next stage of care efficiently, whether that means medical treatment, surgical excision, or Mohs surgery.
Convenience should not be underestimated either. Patients are more likely to stay consistent with preventive care when appointments are available close to home and scheduling is straightforward. Across North Georgia, Goodman Dermatology helps patients access skin exams, biopsies, and advanced skin cancer care through a multi-location practice designed for timely, specialist-level treatment.
The goal is not to scare you
Skin cancer screening is not about assuming the worst every time you notice a spot. It is about taking uncertainty off your shoulders and replacing it with an expert evaluation.
Some appointments end with a simple answer: this is benign, keep an eye on it, come back if it changes. Others lead to treatment at a stage when options are more straightforward and outcomes are better. Both are worthwhile results.
If a lesion has caught your attention more than once, that is usually reason enough to stop guessing and schedule the exam. Peace of mind is useful. Early detection is even better.